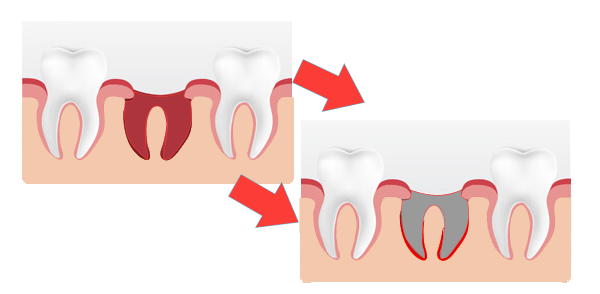
One of the more common complications patients experience after tooth extraction is dry socket. Commonly occurring with wisdom teeth, dry socket is a condition wherein the blood clot that usually stops your gums from bleeding after an extraction becomes dislodged, exposing the bone and nerves and delaying the healing process.
The result is a painful, consistent ache and an increased risk of infection. Not only that, but dry socket can force you to postpone dental treatment to replace the missing tooth.Dry Socket Symptoms & Risk Factors
It’s normal to experience some level of discomfort and bleeding gums after having a tooth extracted. Still, you should start to feel better and begin resuming your normal activities after a few days. If the blood clot doesn’t form, or it becomes dislodged, you may experience increased pain one to three days following your oral surgery. This is telltale sign of dry socket. You may also notice other symptoms, including:
- The socket looks empty or you can see the bone.
- Severe pain, or pain that radiates from your socket to your ear or eye on one side of your face.
- Bad breath or a foul odor or unpleasant taste in your mouth.
- Swollen lymph nodes.
Some dental patients are more likely than others to develop dry socket. Your dentist or oral surgeon can help you determine if you’re at risk for this condition.
For instance, if you smoke you have an increased chance of developing dry socket, so your dentist will normally direct you to stop smoking at least 24 hours before dental surgery. If you have an infection, your dentist will begin tooth or gum disease treatment first to decrease your chance of developing dry socket, or other post-surgery complications.
Women who take oral contraceptives are also more prone to developing dry socket, as high levels of estrogen increase the risk. If you’re taking oral contraceptives, you’ll have a better chance of healing if you have the surgery during the last week of your cycle, when estrogen levels are low.
Finally, if you’ve had dry socket in the past, you’re more likely to get it again. So, it’s important to provide your dentist or oral surgeon with an accurate medical history to help him or her determine the best dental treatment for you.Preventing Dry Socket Syndrome
There are steps you can take to prevent dry socket, both before you undergo oral surgery and as part of your post-operative care.
- Stop smoking at least 24 hours before and 24 hours after the surgery, as tobacco may contaminate the wound site.
- Tell your dentist about any medications you are taking; some medications can interfere with blood clotting.
- Following the surgery, refrain from spitting or using a straw, as the sucking action could dislodge the blood clot.
- Maintain good oral hygiene, but be careful brushing around the extraction site.
- Use a warm saltwater rinse to keep the area clean, but don’t rinse your mouth too vigorously.
- Don’t touch the wound with your fingers or other objects.
- Eat soft foods and avoid foods that could lodge in the wound, such as popcorn, peanuts or pasta.
Dry Socket Treatment
According to WebMD, only about two to five percent of extraction patients develop dry socket. If you are one of them, your best course of action is to immediately contact your dentist.
Your dentist may need to flush out the socket to remove debris and apply medicated dressings to protect the area. Your dentist may also prescribe medication to control your pain. Be sure to follow your self-care advice at home.
Despite the fear some people may have about tooth extractions, if your dentist recommends one, trust that it is in your best interest and in the best interest of your continued oral health.